
Stigma of STDs
Sexually transmitted Diseases come with so many different pseudonyms – The Clap (gonorrhea), The Clam (chlamydia), The Gift that Keeps on giving (herpes), Hi-Five or The Virus (HIV), Syph (syphilis), and Trich (trichomonas). It’s hard to keep track of so many aliases. It makes understanding and breaking down misconceptions and stigmas about STDs more difficult.

But all joking aside, for the majority of people, catching an STD is similar to being sentenced with a lifetime punishment. I can’t begin to tell you how many patients I have encountered, both men and women, who feel exposed and haunted, degraded by not only their peers but by themselves. A mixed bag of emotions is associated with STDs: anger, defeat, confusion, shame, etc.
But! This shouldn’t be the case.
The key to breaking down misconceptions is to understand STDs, and for BOTH men and women to practice prevention!
The purpose of today’s blog is to be that resource. I have broken the blog down into 3 parts or lessons. Feel free to jump to any part you like. As a first aside, I would like to note that HPV is the most commonly transmitted sexual disease, and I will go into greater depth in a separate blog post. I will instead focus on Herpes, Gonorrhea, Chlamydia, and HIV. To better equip you all, I have referenced STDTESTING.ORG, planned Parenthood, the CDC and other major organizations to further enhance YOUR understanding of STDs, how they are tested, and how individuals can better protect themselves to live healthy lives that incorporate safe sex practices. Below is the summary of today’s discussion:
- Breaking down the stigma
- Understanding Disease
- Practicing Prevention
#1 Breaking down the stigma
The greatest issue about STDs is the fact that we have stigmatized it, made it something to fear, rather than something to understand. Sexually transmitted diseases are simply a health issue. The common cold, “food poisoning” or urinary tract infections are either bacterial, viral, or yeast infections that create an inflammatory response in your body. STDs are doing the same. The challenge that arises is that STDs are associated with a personal part of our lives, where individuals are hoping their health is secure with someone they are intimate with. It’s when that intimate trust is violated that we demonize and shame individuals.
The best place to start breaking down stigmas is with your partners. Many loving partners are aware that their partner has an STD. Others do not. The spread of an STD occurs because there is a lack of communication and understanding. According to STD TESTING, “in their early stages, many STDs are largely asymptomatic, which precipitates their spread by unknowing carriers. Sexually active adolescents and young adults (aged 15 to 24) are at particular risk, with nearly 10 million new infections occurring every year.”
So what should you bring to the table when speaking with your partner?


Planned Parenthood put it best “It’s totally normal for the conversation to feel a little awkward, but you’ll feel better once you get it over with. And you never know — your partner might be glad you brought it up.” You are stronger as a cohesive, trusting partnership. This type of vulnerability is healthy and creates trust.
#2 Understanding Disease
I recently posted on my Instagram account @dannynikumd what people would like to know about STDs. Many of the responses circled around a better understanding of STDs, how to understand your test results, and how they affect fertility. Below is an image you can download onto your phone and take to your doctor’s office. I have answered a few of the questions myself!
Where can I get tested? What does a lab test look like?
After the Affordable Care Act was enacted, Most STD testing is now covered or reduced in cost if you have insurance.
Your primary care doctor or your OBGYN will be able to perform the necessary tests in their offices. You can also visit Planned Parenthood for testing as well. STDTESTING.ORG also has a comprehensive website with locations for clinical testing. Click the link below to directly access this.
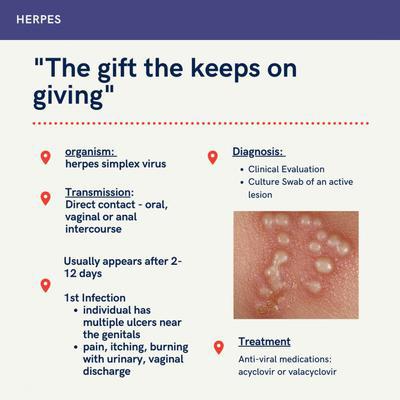
Here is a sample test. This one in particular is pretty comprehensive because it has covered Herpes and Hepatitis C as well. Generally, most STD tests will look for Gonorrhea, Chlamydia, HIV, Syphilis and Hepatitis B. While a blood test can detect if you have antibodies for herpes (meaning you may or may not have been infected by the virus), it doesn’t tell physicians if you have an active infection. That is usually diagnosed when there are genital or oral lesions, and a swab is collected. Therefore Herpes is best detected via culture swabs. Hepatitis C is detected by blood tests and is more commonly tested in high risk populations, such as those with multiple sex partners, exposure to IV drugs, or sex traffickers. The test above for Mr. John Adams is negative.
What happens if I am positive?
Your physician should call you with the results and discuss the next steps, including treatment, precautions and preventative measures (i.e. safe sex practices, avoiding intercourse until the treatment is complete, speaking with your partner). It is important to note that most STDs will need to be reported to government Health agencies.
How do STDs affect my fertility??
Some STDs can affect fertility, specifically gonorrhea and chlamydia. These preventable infections can cause pelvic inflammatory disease, which includes infections to the cervix, uterus and fallopian tubes. If untreated, these organs can develop scarring and block the reproductive organs. For instance, chlamydia and gonorrhea can affect the normal cells of the fallopian tubes. These ciliary cells help move the eggs (embryos) to the uterus for implantation. But with damage to the fallopian tubes, these embryos can get stuck, causing ectopic pregnancies.
Highlighting those STDs:





#3 Practicing Prevention
So, as we know STDs exist, but their spread can be avoidable and prevented. More importantly, having an STD DOES NOT DEFINE YOU. How you manage, understand and prevent the spread of STDs is more characteristic of a smart, altruistic individual.
First and foremost, practice safe sex. Just because you had an STD once and it was treated, does not mean you can’t get it again.
So, what is the best form of contraception to prevent the spread of STDs?
Condoms! While condoms are effective as a birth control method, they are more reliable as barrier protection to STDs.
This is especially important if you plan to have multiple partners! The frequency of partners increases the risk of transmission of STDs.
What are other preventative measures?
- Vaccination against HPV (brands such as gardasil are available and administered for young men and women between the ages of 12-26 years old)
- Speak to your partner (see above)
- Get tested!
It is recommended that women under the age of 25 get screened for STDs (specifically Gonorrhea and Chlamydia) because this STD is more commonly spread in the younger population
We covered a lot of ground today. I hope we were able to: breaking down the hidden stigmas with STDs, understand them a little more clearly, and I hope I have provided a clear way that prevention can be practiced. STDs are on the rise in the US, and this blog I hope will guide us in the right direction.
